News from the Johns Hopkins Hospital Department of Nursing, Johns Hopkins Bayview Medical Center, and Howard County General Hospital (a member of Johns Hopkins Medicine)
Johns Hopkins Hospital Department of Nursing
From Inpatient to Prom Princess
Super-users to the Rescue
Researchers Walk the Fine Lyne
Howard County General Hospital
A Member of Johns Hopkins Medicine
New Pavilion Improves Patient Safety
Johns Hopkins Bayview Medical Center
Suburban Hospital Healthcare System
From Inpatient to Prom Princess
Nurses make a teenager’s prom dream come true
The Pediatric Oncology Unit, CMSC-8, had just rolled out the new Sunrise Provider Order Entry (POE) system. Talk about stressful times! The nurses had plenty on their minds. Were the orders correct? Did the lab labels print accurately? Were they getting this right?
 But amidst the POE rollout, there was something much more important happening on the floor that day: Someone had to get to the senior prom.
But amidst the POE rollout, there was something much more important happening on the floor that day: Someone had to get to the senior prom.
You only have one senior prom in your life. For 18-year-old Vanessa (not her real name), prom was this Saturday–and she wasn’t prepared. How could she be? She had been sick in the hospital for days.
Vanessa was brought to the hospital for diabetes insipidus, which had been caused by the steroids she had been given to reduce a recurrent germ cell tumor. The diabetes was out of control and she needed to get on insulin and be taught how to take care of herself with this new development.
This story probably sounds like a thousand others you have heard. Well, maybe not a thousand stories, but you know–someone needs to go to a prom, they don’t have a dress, someone else supplies it, and “Voila!” they are off to the dance, just like Cinderella herself.
But that is not how this story went, exactly.
Vanessa really wanted to go to her senior prom. Her nurse, Christine Woo, RN, and the resident on duty, Katie Sussman, had a lot to do to get her safely ready for discharge in time for the prom.
Then there was Julia Sussan, RN, the nurse who was the dress champion for the day. When Julie found out that Vanessa wanted to go to the dance, but didn’t have a dress, Julie–who was five months pregnant–said she had a lot of bridesmaid dresses at home. She thought that Vanessa and she were about the same size–at least before she’d become pregnant. Julie volunteered to call her husband Tom, a Hopkins post doc in public health, who was home painting, and who she was sure wouldn’t mind bringing in some of those dresses she had in the closet.
Well, the patient said, that was great, but she wanted a green dress. Only a green dress would do.
Julie thought about it. She had a green bridesmaid dress, but it was a very particular dress, one that Julie didn’t think she could part with.
The green dress was one she had worn in February 2006 as a bridesmaid in the wedding of her dear friend, Catherine. Catherine had cystic fibrosis, and had undergone a double lung transplant here at Hopkins in March 2006. She died later that month.
Julie, along with some of Catherine’s other friends and family, started a foundation called Catherine’s Fund 4 Cystic Fibrosis (CF4CF). In fact, the evening I met Julie, she was wearing her CF4CF tee-shirt under her scrubs. The foundation has raised more than $24,000 since it was started.
Julie had recently been working on cleaning out her closet and had even thought about donating all of those dresses to a charity. All of them, of course, except the green one.
Well, you know how young prom princesses are when they make up their mind on a color. Vanessa didn’t even want to hear about the other dresses once she heard about the green one.
Julie knew that she would never wear the dress again. So she sucked it up, called Tom, and talked him into putting down the paint brush, finding the dress, and carefully bringing it in for the soon-to-be prom princess.
Everyone else went into high gear. Makeup and nail polish were located, a sash was fashioned out of a few pillowcases, decorated with the moniker “Prom Princess.” Even the POE nurses jumped in and helped. All the orders were written, the teaching was done, and off she went to the prom. And, like Cinderella, she was late.
Pediatric oncology nurses see a lot of tragedy. Their stories don’t always have a happy ending. But without a doubt, that night certainly did, as one young lady was transformed from a patient into a princess!
–Stepanie A. Kearns, RN
On prom night, Stephanie Kearns, RN–the writer of this story–was working on The Pediatric Oncology Unit to support the rollout of the new POE clinical documentation system.?”This story involved a lot of giving, a lot of hope, and quite a few Hopkins employees working together to make a young lady’s prom dream come true,” says Kearns. “I was so proud of these nurses and their kindness; it was wonderful to even have the ability to work on their unit to assist them with POE.”
Super-users to the Rescue
Nurse specialists help get diabetes under control
With more than 2,000 nurses and nearly 1,000 beds, the task of improving care for diabetic inpatients at The Johns Hopkins Hospital could seem downright daunting. But with a cadre of Super-users–nurse experts in diabetes management and patient care–on each unit, the situation (and blood sugar levels) are under control.
“The disease can negatively affect a patient’s recovery,” noted nurse practitioner Joanne Dintzis, MSN, CRNP, CDE. “If hospitals don’t improve blood sugar levels of inpatients, they can suffer from wound infections and slower healing after surgery.” And insulin, which is often used to treat the disease, is considered a top-five high-risk drug that, if delivered incorrectly, can lead to death.
Dintzis serves as a clinical facilitator, charged by a taskforce of hospital leaders to improve diabetes care.
In 2006, improving care for diabetic inpatients gained steam after the American Diabetes Association and the American Association of Clinical Endocrinologists released a joint statement calling for improved care of diabetic patients in American hospitals.
That year, the Hopkins taskforce developed a series of workshops to educate nurses about the dangers facing diabetic inpatients whose blood sugar is insufficiently monitored. But the workshops were reaching a tiny fraction of the nurses. “It was a good turnout,” said Dintzis, “but we still had an awful lot of nurses we were not reaching.”
That’s when the taskforce conceived the idea of Super-users.
Each of the hospital’s more than 40 care units has now committed at least one nurse to help educate other nurses about properly managing diabetes. Currently Hopkins has 90 Super-users, and the program is widely successful.
“We help the Super-users understand the hospital policies associated with diabetes care, and then they can be our liaisons with the staff on their units,” Dintzis said. “We’re really focused on keeping the patient safe and avoiding harm because it is a dangerous disease.”
-Lester Davis
Researchers Walk the Fine Lyne
With grants from the Dorothy Evans Lyne Fund, Hopkins nurses–from the hospital and the school–are partnering on research to improve patient care
Valid and Reliable? Nurses Assess the Johns Hopkins Fall Risk Tool
You may think that nurses at The Johns Hopkins Hospital are a bit overzealous in their devotion to studying and preventing inpatient falls. Then again, if you know that falls are the sixth leading cause of injury and death among inpatients, you might admire their spirit of inquiry and determination.
 Hopkins nurses first developed a tool to assess and prevent patient falls back in 2003, said Patricia Dawson, MSN, RN, who helps coordinate the fall risk program. Today, it is used in all adult inpatient units at Johns Hopkins and has been embraced by more than 50 other hospitals in the U.S. and around the globe.
Hopkins nurses first developed a tool to assess and prevent patient falls back in 2003, said Patricia Dawson, MSN, RN, who helps coordinate the fall risk program. Today, it is used in all adult inpatient units at Johns Hopkins and has been embraced by more than 50 other hospitals in the U.S. and around the globe.
Because the tool has been adopted by so many clinicians, the Hopkins nurses decided to make sure the tool was measuring what it was designed to measure–fall risk. This required a rigorous study, so the nurses applied for a grant from the Dorothy Evans Lyne (DEL) Fund to test its reliability and validity. Like all research funded by DEL, the fall risk study is being conducted jointly between a team of nurses from the hospital and Johns Hopkins University School of Nursing.
Members include Stephanie Poe, MScN, RN, assistant director of nursing of clinical quality and informatics; Patty Dawson, MSN, RN, coordinator for Magnet and quality; Maria Cvach, MSN, RN, assistant director of nursing clinical standards; Margie Burnett, BSN, RN, NCIII; Linda Costa, PhD, RN, nurse researcher; and Elizabeth Hill, PhD, RN, Assistant Professor at the school of nursing.
“The school of nursing has really reached out to the hospital to help them with real life issues that the nurses are faced with on a daily basis,” said Cvach, assistant director of nursing and clinical standards for Central Nursing Administration. “They’re not just teaching the students to do research. The school of nursing is interested in solving some real life issues that we face at the hospital.”
In the summer and fall of 2009, nurses at Hopkins have been gathering information on more than 1,600 inpatients. Within two hours of admission, adult inpatients are assessed by a nurse, who looks at factors such as age, type of medication, and use of cumbersome hospital equipment (like an IV pole) that might increase the risk of a patient fall. Each patient in the study receives at least four assessments, which are then compiled by a researcher.
It’s too early to glean any information from the data that have been collected so far, says Cvach, but when the study is completed next summer, nurses may have a proven tool to help these at-risk patients.
Teach-back to Reduce Readmission
With little follow-up or guidance after hospital discharge, it’s no wonder that the 30-day readmission rate for U.S. heart failure patients hovers around 25 percent.
To keep heart failure patients out of the hospital, nurses at The Johns Hopkins Hospital knew that patients must be given the right information–in a way they could understand and remember it.
 As part of a DEL-funded pilot, nurses launched the so-called “teach-back” method to improve care transitions. Team members from The Johns Hopkins Hospital were JoAnn Ioannou, MSN, MBA, RN, assistant director of medical nursing; Stacey Rotman, MSN, RN, heart failure care coordinator; Kelly Caslin, RN, nurse manager; and Karen Davis, MSN, RN, director of medical nursing. The principal investigator, Cheryl Dennison, PhD, ANP, and Jerilyn Allen, ScD, RN, joined the team from the School of Nursing, and Stuart Russell, MD, associate professor at the School of Medicine was also on board.
As part of a DEL-funded pilot, nurses launched the so-called “teach-back” method to improve care transitions. Team members from The Johns Hopkins Hospital were JoAnn Ioannou, MSN, MBA, RN, assistant director of medical nursing; Stacey Rotman, MSN, RN, heart failure care coordinator; Kelly Caslin, RN, nurse manager; and Karen Davis, MSN, RN, director of medical nursing. The principal investigator, Cheryl Dennison, PhD, ANP, and Jerilyn Allen, ScD, RN, joined the team from the School of Nursing, and Stuart Russell, MD, associate professor at the School of Medicine was also on board.
Teach-back starts in the hospital, when a nurse explains disease management, such as signs and symptoms, nutrition, medications and appointments. The patient repeats the information (“teaching back”) to the nurse, which gives them a chance to clear up any confusion.
Within five days of discharge, a nurse calls the patient at home to check in and assess the retention of the lesson. Two weeks later in the clinic, the patient will again go over the disease information.
“We want to reduce readmission rates, and we want to improve quality of life for patients,” said Ioannou. A patient who understands and is engaged in his care, Ioannou adds, can better manage the disease.
Although they have seen a “significant difference in readmissions,” Ioannou said it’s too early to tell if it’s directly related to the teach-back program.
The initial pilot, which ran from January to May 2009, included 157 patients for a total of 225 admissions. About half of those admissions received call-backs or clinic visits, and of those, just 10 percent were readmitted within 30 days of discharge, according to Ioannou’s data.
-Lester Davis
The Dorothy Evans Lyne Fund
The DEL fund supports pilot studies conducted by teams of nurses from The Johns Hopkins Hospital and Johns Hopkins University School of Nursing. Each study is designed to improve patient care and outcomes, provide evidence to validate clinical practice, or examine the effectiveness of clinical care delivery systems.
The fund was established in 2001 by June R. Elliott, a grateful Hopkins patient, in honor of her long-time friend and Hopkins nursing alumna, Dorothy Evans Lyne ’59.
Emma Barth, House Hunter
Hopkins nurse find her dream home on reality TV
Emma Barth, RN, spent two years touring dozens of houses in the search for her dream home. She’d still not had success when producers from HGTV’s House Hunters approached her real estate agent about appearing on the reality show.
 “We thought it would be a fun experience,” said Barth, a nurse clinician at The Johns Hopkins Hospital.
“We thought it would be a fun experience,” said Barth, a nurse clinician at The Johns Hopkins Hospital.
Newly married and renting in Baltimore’s Charles Village neighborhood, Barth cast her house-hunting net on the Canton area. Shooting for the program began in late May, and Barth and her real estate agent visited up to a dozen houses in a single day.
Almost immediately, Barth realized she had agreed to more than she bargained for. “It was a painstaking process,” she said, adding that the show’s producers had her focus on the more peripheral aspects of each house she visited, like paint color or the molding around stairs.
Being on the show, said Barth, “was a total eye-opener to the ways of reality television. I don’t think I would do it over again now that I know what the process is like.”
After several days of shooting and missed time at work–Barth found the perfect two-bedroom, 1,300 square-foot row house in Canton. The house, says Barth, fit her checklist of must-haves: open design, new appliances, and spacious backyard. She and her husband moved in June 1, 2009.
The segment is scheduled to air around March 2010. If you miss the show on TV, you can watch it online at www.hgtv.com/house-hunters/show/index.html.
–Lester Davis
Satisfaction on the Job
Surveys show that Hopkins is a good place to be a nurse
“Job satisfaction is a key factor in attracting and retaining the best nurses,” according to Patty Dawson, MSN, RN, coordinator for Magnet and Quality for The Johns Hopkins Hospital. That’s why this June, more than 70 percent of the hospital’s nurses participated in two surveys to gauge their satisfaction and engagement in the workplace.
Among the 7,300 hospital employees who took the Gallup Q12 employee engagement survey were 1,700 bedside nurses. A more engaged nursing staff can mean improved efficiency, patient satisfaction, and safety, so with nurses comprising approximately 23 percent of Hopkins’ workforce, their participation in the survey was important.
 “Our employees are our most valuable asset, and we want to have a way to capture their feedback,” said Carol Woodward, a Johns Hopkins human resources consultant who helps coordinate the Q12 survey every two years. The results for nurses showed improvement over the 2007 “Grand Mean” score as well as scores in 10 of the 12 individual questions on the survey, Woodward said.
“Our employees are our most valuable asset, and we want to have a way to capture their feedback,” said Carol Woodward, a Johns Hopkins human resources consultant who helps coordinate the Q12 survey every two years. The results for nurses showed improvement over the 2007 “Grand Mean” score as well as scores in 10 of the 12 individual questions on the survey, Woodward said.
The RN Job Satisfaction survey, administered through the National Database for Nursing Quality Indicators and coordinated at Hopkins by Dawson, measures nurses’ satisfaction with their level of input in decision-making, time to complete tasks, overall job enjoyment, and perceptions about quality of care. Results from 2005, 2007, and 2009 have revealed consistent improvement in all four areas–and Hopkins remains above the national average.
Managers are sharing the survey data with nurses on their units this fall. Together, they will work to assess the unit’s strengths and plan for continued improvements to make Hopkins an even better place to be a nurse.
New Pavilion Improves Patient Safety
Nurses offer ideas on room design for hospital’s new inpatient addition
Interior design requires a different skill set from providing bedside care. Nurses aren’t trained to read blueprints or to work with architects and electricians. And yet, the nursing staff at the Johns Hopkins Medicine-affiliated Howard County General Hospital (HCGH) played an important role in planning the hospital’s new 90-bed inpatient pavilion, which opened August 3.
 The collaboration made sense for several reasons. Patient safety and improved quality of care were the driving forces behind the new addition. Nurses are in daily contact with the clinical needs and wishes of patients and their families. They know what works in a hospital setting and how small changes, such as the placement of a chair, or significant ones, like having private rooms, could work better for patients and staff.
The collaboration made sense for several reasons. Patient safety and improved quality of care were the driving forces behind the new addition. Nurses are in daily contact with the clinical needs and wishes of patients and their families. They know what works in a hospital setting and how small changes, such as the placement of a chair, or significant ones, like having private rooms, could work better for patients and staff.
Doree Turnage, RN, PCCN, clinical program manager for the new 3 Pavilion, participated in a committee of nurses that met regularly to offer ideas and feedback on room design to Beth Plavner, HCGH’s special projects administrator who was in charge of overall planning for the new four-story pavilion. “Safety was a first concern,” said Turnage, whose unit cares for a wide variety of illnesses from stable ventilator patients to those in need of pulmonary, renal, and surgical care. Many of these patients are elderly. One outcome of these planning meetings: bathrooms in the new pavilion feature elevated commodes with side railings for ease of use. To decrease the risk of falls, safety railings were installed at strategic locations to assist patients in getting to the bathroom safely.
The nurses also wanted to make sure there was adequate clearance for their carts and equipment to navigate the hallways and patients’ rooms. “Beth constructed a mockup room so that the staff could offer their concerns and opinions,” said Turnage. “We also wanted enough space to accommodate family members who are visiting or spending the night. Having a family member present is very reassuring to an elderly patient. As a result, each inpatient room has a sleep sofa, a desk large enough for a laptop, shelving for personal items, and a closet.”
The new addition contains three new 30-bed inpatient units, all with private rooms. Private rooms reflect a trend in hospital design since the introduction of HIPAA, the federal privacy law, Turnage explained. This trend also helps reduce patient infection because it lowers the risk of cross-contamination that could occur from having a roommate.
Reducing medication errors was also a priority for the hospital. One solution the nurses came up with was to keep each patient’s medications in an alcove outside his or her room. Each alcove in the new pavilion contains a place for the nurse to sit at a computer to take notes and monitor the patient’s heart rhythms on a telemetry screen. This arrangement is “nurse friendly,” said Jacqueline O’Neale, RN, a staff nurse on 2 Pavilion, who participated in a feedback session on the prototype room design. O’Neale and her colleagues suggested that each alcove house a locked drawer for each patient’s medications and a cabinet above the desk be set aside for storing supplies such as tissues, bedpans and urinals.
“All the nurses like the new room design and the alcoves,” said O’Neale. “We can sit at the desk and do our work. We don’t have to be at the nurses’ station.”
“The patients like it too,” said Turnage. “Each room has calming colors, a large window, and artwork hanging above each bed. The rooms are light-filled, clean, and quiet, which is more restful for the patients and consequently less stressful for the staff.” One patient recently commented that she had donated to the hospital and it was very nice to see her donation go to such good use, Turnage said.
–Susan Middaugh
Beat the Clock
CICU nurses cross-train for quicker angioplasties
Two years ago, the nurses in the Cardiac Intensive Care Unit (CICU) at Johns Hopkins Bayview Medical Center wanted to improve the chances of survival for patients experiencing chest pain and in need of angioplasty. In doing so, they had to “beat the clock” and extend themselves in unfamiliar ways.
 The clock starts when acute myocardial infarction (MI) patients enter the emergency department for diagnosis and referral and ends in the catherization lab. The state standard for door to balloon inflation time is 120 minutes. Bayview was taking slightly longer than that, but aspired to a more ambitious goal. “We wanted to go by the American Heart Association’s 90-minute standard because that was better for patients,” said Tim McFeely, RN, patient care manager of the CICU.
The clock starts when acute myocardial infarction (MI) patients enter the emergency department for diagnosis and referral and ends in the catherization lab. The state standard for door to balloon inflation time is 120 minutes. Bayview was taking slightly longer than that, but aspired to a more ambitious goal. “We wanted to go by the American Heart Association’s 90-minute standard because that was better for patients,” said Tim McFeely, RN, patient care manager of the CICU.
Closing that gap required ingenuity on the part of the CICU nurses and more than a little juggling. In addition to providing patient care on their unit, these nurses are responsible for codes, a hypothermia protocol for patients following arrest, and serving on a rapid response team. Then they added one more task. Eighteen CICU nurses out of a staff of 35 volunteered to be part of a “bridge” team to be cross-trained in the cath lab.
Here’s how the new procedure works. When a patient with acute MI comes into the emergency department, the CICU nurse goes downstairs to the ER to transport the patient to the cath lab. While waiting for other members of the team to arrive, this nurse stabilizes and preps the patient according to the lab’s protocols, remains present throughout the procedure, and then transports the patient to the CICU.
The bridge team began as a pilot in June of 2007. Since then, approximately 110 men and women have gone through this regimen, said McFeely, noting that “almost immediately we saw a huge improvement” in both the patients’ health and the nurses’ response time. In July 2009, the median door to balloon time at Bayview had been reduced to 70 minutes. “These patients used to be very sick,” said McFeely, “now they’re usually in the CICU for just one day.”
The bridge team has been a win-win for patients and nurses alike, says Heather Wilkerson, RN, CCRN, an advanced clinical nurse educator for the CICU.
Wilkerson and cardiac cath lab nurse Jeff Burkins, RN, trained their colleagues in the new procedure. “The nurses love it,” she said. “It makes them feel empowered, like they’re doing something worthwhile for the patient. In the past many of our acute MI patients died or suffered a poor quality of life after discharge and were frequently readmitted to the hospital. Now many of our acute MI patients walk out of here with their families. They may need to make lifestyle changes, but their outcomes are much improved.”
The nurses have benefited in other ways, says Wilkerson. “They’ve enhanced their skill set by developing a certain level of competency in two different entities of the hospital.”
Janet McIntyre, MSN, RN, CPHQ, senior director of quality and patient safety at Bayview, was so impressed with the CICU nursing team’s efforts to “go well beyond the call of duty” that she nominated them for a regional award from Advance for Nurses magazine. The CICU nurses earned best in initiative and second overall for the best nursing team.
–Susan Middaugh
Overseas Delivery
Thanks to these Bayview nurses, an Air Force dad was able to coach his wife through labor–from Afghanistan
Obstetrics nurses at Johns Hopkins Bayview Medical Center pride themselves on creating a personalized care plan for their maternity patients that combines compassion and expertise with sophisticated technology. But earlier this year Christy McPheeters, RN, received an unusual request from her supervisor. Joe Burns wanted to be with his wife, Amy (not their real names), during the birth of their first child, but he was stationed in Afghanistan with the U.S. Air Force. Could the maternity unit reach out to him electronically?
 McPheeters was recruited for this special assignment because her husband also serves in the Air Force and frequently gets called overseas. “We try to accommodate all of our patients,” McPheeters said, “but this was the first time we had ever done a telecast delivery.” She describes the experience as new and exciting for her and an example of how accommodating the nursing staff is to its maternity patients.
McPheeters was recruited for this special assignment because her husband also serves in the Air Force and frequently gets called overseas. “We try to accommodate all of our patients,” McPheeters said, “but this was the first time we had ever done a telecast delivery.” She describes the experience as new and exciting for her and an example of how accommodating the nursing staff is to its maternity patients.
The Freedom Calls Foundation, a nonprofit in Morristown, N.J., that offers free phone and video conferencing to U.S. troops, helped with the logistics. They arranged for Joe to be in a hotel conference center in Afghanistan where he could be connected to his wife in real time. The hospital supplied the television, a web cam that rotated 360 degrees, a speaker, remote control, and a microphone for Amy.
McPheeters admits that the presence of a TV camera in the labor and delivery room was an adjustment for her. Otherwise, her role was the same–being supportive of the patient, helping Amy push when appropriate and taking care of the new baby. Although the expectant father was physically thousands of miles away, his voice and persona were felt during his wife’s labor because of the video transmission and telephone hookup. The Air Force dad “was very personable and comfortable with the situation,” McPheeters said, which also helped her and Amy. “The couple were able to see and talk to each other” during what could have been an especially stressful event. The only complication was that the induction took longer than Freedom Calls had allotted. As a result, the new dad was no longer available by telecast, but he was able to be on the phone for the birth and able to take still photos of his new baby after the delivery. “The parents were very happy and grateful to have more than eight hours to spend together,” McPheeters said.
About six weeks later, the couple and their newborn returned to Bayview to express their thanks to McPheeters in person. Since then, the maternity unit has received a second request for the same service from an expectant mother who wants her husband, who is stationed overseas, to participate in the birth of their child–remotely. “We try to meet the needs of all of our patients,” said McPheeters. “But it’s nice to know that these options are available to military families.”
–Susan Middaugh
Emergency Accommodation
New Procedures reduce emergency department closures by 50 percent
When the State of Maryland approved Suburban Hospital’s cardiac surgery program a few years ago, the hospital knew it had to be open to as many ambulance patients as possible. The problem was, Suburban’s emergency department (ED) was frequently overwhelmed and often had to close its doors to all but the most severe trauma cases.
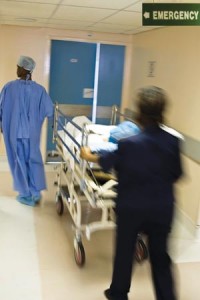 Two years ago those closures started to decline when the nursing staff initiated a patient-centered change in procedure that requires the cooperation of nearly the entire hospital. One of the motivators was a need to be more community-minded.
Two years ago those closures started to decline when the nursing staff initiated a patient-centered change in procedure that requires the cooperation of nearly the entire hospital. One of the motivators was a need to be more community-minded.
Diverting ambulances away from the hospital meant “we weren’t there for the public,” said Cindy Notobartolo, RN, corporate director of Suburban’s emergency/trauma, safety, and security services. “Their doctor and medical records might be here, but they had to go further away to another hospital.” The nurses at Suburban thought they could do better.
The new procedure, called Code C, consists of a comprehensive plan to improve the flow of patients from the ED–which can accommodate approximately 50 patients–to inpatient beds. Of all Suburban’s admissions, 75 percent come through the ED.
“We looked at best practices and principles espoused by the Institute for Healthcare Improvement,” said Notobartolo, “then we fashioned our own protocol.” Interdepartmental cooperation and communication are at its core.
The decision to begin a pre-closure alert rests with the ED’s charge nurse, who is “often in the best possible spot” to assess the situation, said staff nurse Mary Welsh, RN, TNCC, CCRN, PHN, who also serves as a relief charge nurse. An RN for the past 24 years, Welsh has worked in Suburban’s ED for the past six. The goal of Code C, she explained, is to prevent a closure by paging a team that includes representatives from nursing, the ICU, and CCU as well as Admitting, Housekeeping, and Transport Services. Everyone gathers in the ED to discuss next steps. Through an exchange of information and subsequent deployment of staff to different parts of the hospital, a closing may be averted. For example, the cardio-thoracic unit might be able to accept a patient from the ED on a temporary basis. Another patient’s admission might be sped up because Housekeeping dispatches a staff member to clean a recently unoccupied room.
Because of Code C “we now have a shorter prep time for moving patients from the ED to another floor,” Welsh said, “and we’re closing the ED less often.” During the last fiscal year, which ended June 30, for example, Suburban had reduced the number of ED closures by 50 percent, said Notobartolo.
The new system is better for patients, said Welsh. “They don’t have to go to a hospital where the doctor doesn’t know them and is further away for their families to visit.”
Notobartolo agreed. “Our patient satisfaction scores are up and a recent poll of area physicians in Washingtonian magazine indicated that Suburban Hospital was one of the best hospitals to go to,” she said.
–Susan Middaugh
 Alumni Profiles
Alumni Profiles Gatorade, Free of Charge
Gatorade, Free of Charge Jerilyn Allen Receives NIH Honors
Jerilyn Allen Receives NIH Honors Who Wants to Be a Nurse? PhDs and Lawyers, Among Others!
Who Wants to Be a Nurse? PhDs and Lawyers, Among Others! An Eye-Catching Class T-Shirt
An Eye-Catching Class T-Shirt







