Each year, as many as 2,000 children become long-term cancer survivors thanks to a powerful treatment tool: bone marrow transplantation, or BMT. However, this aggressive treatment, when successful in defeating the cancer, is known to come with potential long-term damage to a child’s bones. Without intervention, the damage can lead to considerable pain and disability later in life.
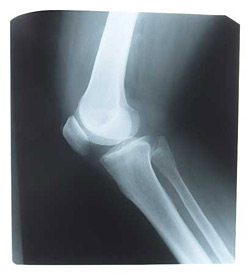
Writing in the Journal of Pediatric Oncology Nursing, Johns Hopkins University School of Nursing clinical instructor and PhD candidate Kathy Ruble, MSN, RN, describes the incidence, risks for occurrence, and symptoms of three of the most salient bone problems that occur in the decades following successful bone marrow transplantation among young cancer patients. They include bony lesions on the skeleton called osteochondromas that can cause pain or restrict movement; thinning bones that can lead to fractures; and avascular necrosis, the death of bone tissue that leads to bone collapse, most often in the knee, shoulder, or hip.
“Oncology nurses are leading the way in the care of cancer survivors and play a critical role in ensuring the best possible outcomes for these individuals,” Ruble observes. She recommends the steps oncology nurses can play in the early identification and treatment of these potentially disabling conditions during routine care of long-term survivors of childhood cancer. Careful review of each patient’s individual risks for these BMT complications, coupled with ongoing monitoring, diagnosis and treatment (including behavioral, pharmacological and physiological interventions) can help promote healthier lives for thousands of young cancer survivors.
 Team Spirits are SOARING
Team Spirits are SOARING In Trouble Before They Even Get Started
In Trouble Before They Even Get Started Nurturing Nursing’s Diversity
Nurturing Nursing’s Diversity Nurse Appreciation is a Two-Way Street
Nurse Appreciation is a Two-Way Street







