Move to bedside report increases patient safety and nurse satisfaction
When Ammini Ninan, MSN, CMSRN, proposed moving change-of-shift report from the nurses’ station and break room to patients’ bedsides, her colleagues on Med B thought she was nuts.
For years, they’d shared information about patients and their care in huddles, away from the eyes and ears of patients. They spent the first 30 to 45 minutes of each shift exchanging information, then went forth to care for their patients. Ninan’s proposal–to include patients and do report nurse to nurse, room to room, bedside to bedside–was a drastic departure from their usual procedure.
[pullquote]
“We took a vote, and the vote was 100 percent in favor,” Applegate says. “It wasn’t, ‘Should we do this?’ but ‘When do we start?’ ” -Michele Applegate, MSN, RN, NE-BC
[/pullquote]
But Ninan, then a student in her MSN program, knew that the evidence was solid. Bedside report has been linked to increased patient safety and patient and nurse satisfaction. Units that have implemented bedside reporting often note a decrease in patient falls, a decrease in medication errors, and an increased sense of inclusion among patient and family members–without increasing nurse stress or overtime.
Michele Applegate, MSN, RN, NE-BC, nurse manager of Med B, was intrigued by Ninan’s proposal and told her to take it before the unit’s Shared Decision Making Committee. At the time, most nurses on the unit were adamantly opposed to the idea. Their thinking, Applegate says, was “that will never work.”
Ninan met the objections head-on. She brought a PowerPoint presentation and articles showing the effectiveness of bedside reporting to the meeting; she also showed the group YouTube videos of nurses demonstrating bedside report.

“By the time she finished her presentation, we took a vote, and the vote was 100 percent in favor,” Applegate says. “It wasn’t, ‘Should we do this?’ but ‘When do we start?’ ”
That was a little over a year ago. In June 2013, after months of preparation, Med B launched bedside report.
The groundwork prior to the official launch was crucial. In order to assure patients’ privacy, the nurses created a report sheet template. The template includes the patient’s past medical history, current diagnoses, and details of care, including test and lab results. Nurses fill out one report sheet for each patient, beginning on admission, and privately and silently share the report sheet outside of patients’ rooms before beginning the “bedside” part of bedside reporting.
Patient care techs also do rounds about 45 minutes before change of shift, helping patients to the bathroom and tending to their needs so they are ready to participate in report. (Nurses also offer pain meds before change of shift.)

The unit also adjusted charge nurses’ hours; they now come in (and leave) a half hour earlier than bedside nurses, so they can provide patient coverage while the nurses move from bed to bed.
During report, the outgoing nurse introduces the incoming nurse to the patient. Together with the patient, they discuss the plan of care for the shift. The nurses also check the patient’s IV site, lines, and fluids, assess pain control, and perform an overall safety check.
Med B staff quickly realized that bedside report fit well into their Comprehensive Unit Safety Program (CUSP). “Previously, most of our staff was tied up for the first 30 minutes of a shift,” Applegate says. “Now, they’re right there in patient rooms. If something is wrong, they’re going to be able to catch it.”
Three months after starting bedside reporting, patient satisfaction scores were up and “nurse satisfaction scores were 100 percent,” Ninan says. One year later, satisfaction scores remain high, Ninan has been named Bayview’s Nurse of the Year and representatives of Med B are preparing to present a poster detailing their experience with bedside reporting at the 2014 Academy of Medical–Surgical Nursing conference.
“Everybody is happy,” Ninan says.
Photography by Chris Hartlove

 A Letter from Deborah Baker: The Role of Your Career, Right Here
A Letter from Deborah Baker: The Role of Your Career, Right Here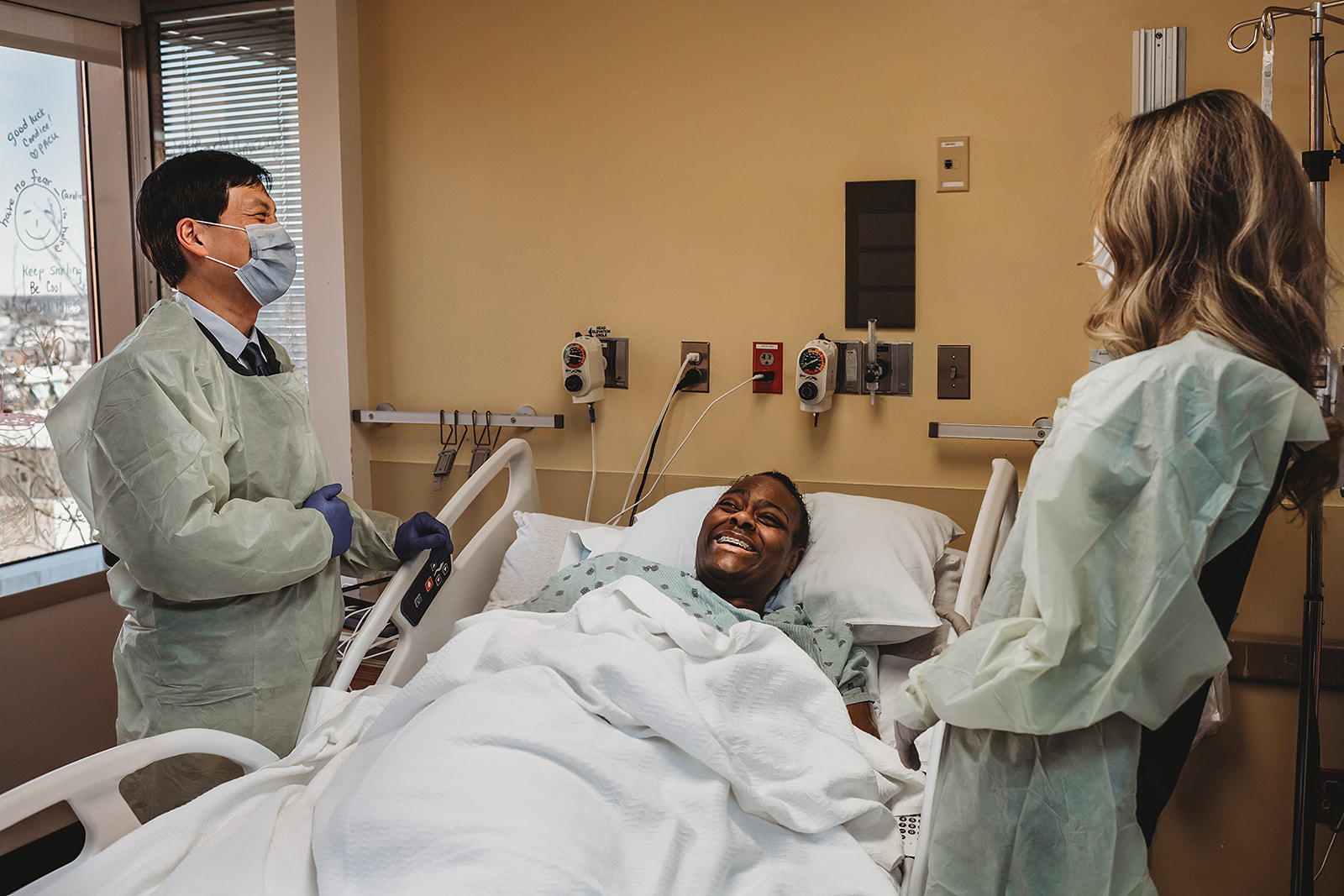 ‘Helpful, Powerful, Kind’ Palliative Care
‘Helpful, Powerful, Kind’ Palliative Care A Tested Tool Keeps Patients Safe
A Tested Tool Keeps Patients Safe DAISY Awards
DAISY Awards Certifiably Awesome
Certifiably Awesome







