Story by Michael Anft
Photos by Bill Denison
Through their holistic approach to health, Hopkins nursing students are improving the lives of countless schoolchildren—and their families—in Baltimore’s underserved communities.
 It’s just past lunch period at St. Bernardine’s Catholic School when a 5th-grader named Dayonna limps into a classroom that has been converted into a nurse’s suite. Her thigh aches. “I hurt it twice playing dodge ball, once when I got hit by the ball, and again when I tried to move it,” she explains.
It’s just past lunch period at St. Bernardine’s Catholic School when a 5th-grader named Dayonna limps into a classroom that has been converted into a nurse’s suite. Her thigh aches. “I hurt it twice playing dodge ball, once when I got hit by the ball, and again when I tried to move it,” she explains.
Like many students at urban parochial schools across the country, Dayonna walks each day into a building that shows signs of wear—halls that need painting, a broken window that resembles a crystalline spider web and hasn’t been replaced. St. Bernardine’s, in southwest Baltimore, is cash-strapped. Too often, students like Dayonna aren’t able to receive health care during classes—save, perhaps, for an aspirin or two offered by a school secretary.
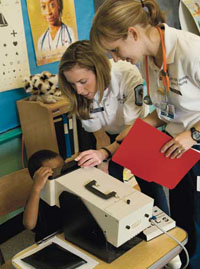
Fortunately for the 225 children who attend kindergarten through 8th grade at St. Bernardine’s, students and faculty from Johns Hopkins University School of Nursing (JHUSON) have, for the past decade, regularly provided them with basic nursing services and health education. As part of one of several partnerships the SON maintains with local public and private schools in underprivileged neighborhoods, nursing students spend much of their afternoon testing uniformed children for blood pressure, hearing, and vision problems; measuring height and weight as a way to monitor obesity; and tending to asthma attacks, bumps, and scrapes. And dodge ball injuries.
Today, under the direction of assistant professor Maureen C. Maguire, MS, RN, PNP, one of four students who are working in the nurse’s office as part of a Nursing for Child Health course takes Dayonna’s case. The student, Kyle Blount, gives her a cold pack, makes up one of the suite’s beds for her, checks her records to see what medicines he is allowed to administer, and then crushes up an aspirin because, she says, she can’t swallow whole pills.

While brushing up on their basic skills, says Maguire, nursing students learn how to handle children, measure basically healthy children against the unhealthy ones many will likely see suffering in hospitals, and get a chance to understand the problems of communities where they might one day work. They also serve, mostly unwittingly, as role models.
“The nursing students are very popular with the children,” says Maguire, of the Department of Community and Public Health. “The kids are definitely not scared to come here. They look up to them.”
“As is the case with many of JHUSON’s community partnerships, its commitment to St. Bernardine’s is multifaceted. Later in the fall semester, graduate nursing students will perform complete physical exams on elementary school students whose parents have signed up for them. And SON faculty and students teach classes on everything from how to handle bullying to hand washing to life skills, utilizing teaching methods that attempt to engage youngsters through role playing and games.
With the help of the children, the nursing students lead extra-curricular activities, including an annual six- to eight-mile walkathon that alerts youngsters to the benefits of exercise.
“We started it three years ago as a competition, but the kids didn’t really take to that,” says assistant professor Sara Groves, DrPH, MPH, MS, RN, CS. “They liked the idea of setting their own goals and trying to achieve them. By listening to the kids, we were able to come up with something they could get excited about.”
Reaching out to children in under-served neighborhoods is exciting for many nursing students as well. Some of them hope to make careers out of serving such communities. “That’s one of the big reasons I decided to come to Hopkins,” says Robin Patch, one of the nursing students at St. Bernardine’s and formerly a psychotherapist in Brattleboro, VT. “I knew there’d be a lot of opportunities to do this kind of work.”

Each semester, 50 or more JHUSON students, some of them former Peace Corps volunteers, strike out into the surrounding community to further their education and be of service. But in a city where one in four people lives in poverty, the nursing students need to be sensitive to the issues they face once they hit the streets, schools, or clinics. There are some lessons they need to learn in the classroom first. Near the end of a late summer day, more than 50 students file into a lecture hall at the Anne M. Pinkard Building to learn what they’re likely to hear about Johns Hopkins from its neighbors. Too often they’re not singing its praises.
Five painted images of legendary Hopkins nurses from the past san-guinely watch over students in the Community Outreach to Underserved and Vulnerable Communities in Urban Baltimore class as guest speaker Adrian Mosley, an administrator in the Medical Institutions’ Office of Community Health, gives students the word on the street.
People in predominantly African-American East Baltimore remember that Hopkins wasn’t desegregated until the 1950s, Mosley notes, and that several community development schemes during the intervening years have fallen short of their goals, leaving the area in even worse shape than it was before good intentions became dashed by hard economic realities.
“The perception is that Hopkins is this 800-pound gorilla that keeps eating its way through the community,” says Mosley. Although her lecture is mostly cautionary, she does leave the students with something positive: “People in the community don’t like Hopkins, but they trust people from Hopkins,” she says.

Once students have finished the one-credit, nine-week course in the fall, they can try to gain the community’s trust by working at several organizations with which JHUSON has created partnerships, including a home for battered women, a clinic, and a high-rise building for the elderly.
“The way we approach all of these collaborations is to understand the strengths the community has, and how the JHUSON brings separate strengths,” says associate professor Nancy Glass, PhD, MPH, RN. “Together, these strengths can be leveraged to bring additional resources and power to the community.” The process starts by allowing community members to “define the issues they consider most important,” Glass notes.
In her work with intimate partner violence, for example, she’s found that violence prevention is often not her clients’ top priority. The women she meets at shelters and clinics have more pressing concerns: finding housing, figuring out how to get custody of their children, getting a job. “We have to be flexible and understanding,” says Glass. “We have to work with people where they are and meet their basic needs first. We must define health broadly.”
That’s exactly the approach nursing students take at Tench Tilghman Elementary, a school four blocks east of the Medical Institutions where 91 percent of the youngsters are eligible for free lunches.
In conjunction with the Julie Community Center, a charity run by a Catholic sisterhood, nursing students help Tench Tilghman students who suffer from asthma, behavioral problems, and poor nutrition. They teach classes on sex education and substance abuse. They offer “health promoter training” to parents they meet on the sidewalk outside school. They refer children who need health care to providers who accept federal or state assistance payments. And they perform the functions of a school nurse in a school that doesn’t have one, owing to a cash-poor city health department.
“This type of collaboration is a two-way street,” says Joshua Sharfstein, the city’s health commissioner. “Nursing students gain practical experience and our students benefit from extra care.”
Sharfstein adds that the high quality of work done by the School’s nursing students will factor into the health care of young children and their families at a new school being built as part of a massive redevelopment plan now under way for the neighborhoods surrounding the East Baltimore Hopkins campus. “The Johns Hopkins University School of Nursing is a great resource in Baltimore, and we would pursue any opportunities for increased collaboration,” Sharfstein says.
For Glass and other community health faculty, the important message to the School’s nursing students is: “People deserve quality health care wherever they go.” She adds, “We try to make it as comfortable for clients as possible, and be as respectful as possible. And we try to model that for our students so that when they go out to practice in the community, they’ll understand the complex issues these patients face and avoid creating artificial barriers.”
 Outsized Influence
Outsized Influence Bloomberg Distinguished Professor Brings Expertise on Disparities and Childhood Obesity
Bloomberg Distinguished Professor Brings Expertise on Disparities and Childhood Obesity Kids are bigger coronavirus spreaders than many doctors realized
Kids are bigger coronavirus spreaders than many doctors realized Getting Curious with Jonathan Van Ness… and Dr. Brittany Wenniserí:iostha Jock
Getting Curious with Jonathan Van Ness… and Dr. Brittany Wenniserí:iostha Jock Knowledge Gap at the Heart of VAD Care
Knowledge Gap at the Heart of VAD Care







