By Lester Davis
Sidney Kimmel Cancer Center offers patients a lovely place to heal
Jacqueline Dunford, who long dreamed of spending her retirement closer to her adult son and grandchildren, breathed a sigh of relief in early June after moving from her hometown of Norfolk, Va., to a house in Federal Hill. With a new job lined up and family nearby, Dunford, 56, couldn’t believe how quickly her plans had come together. She was just beginning to settle into her adopted

At the Sidney Kimmel Cancer Center on the Johns Hopkins Bayview campus, nurses’ fingerprints are all over the thoughtful details.
hometown and was set to begin work as a data analyst at Johns Hopkins Bayview Medical Center when a regular visit to the doctor in July “rocked my world,” Dunford said.
Results from a routine check of her bloodwork indicated a recurrence of the breast cancer she’d spent the better part of 2014 battling. “We kind of had to go backwards and start all over,” Dunford said.
The physical space here is beautiful. I have more privacy, which is huge when you have to sit for hours to receive treatment.”
— Jacqueline Dunford
While the Norfolk facility, where she was treated last year, lacked adequate privacy, and was located in a non-descript strip mall, the recently-opened Sidney Kimmel Cancer Center on the Johns Hopkins Bayview campus offers Dunford “expert attention to detail and state-of-the-art equipment.”
“The physical space here is beautiful. I have more privacy, which is huge when you have to sit for hours to receive treatment,” Dunford said.
Her reaction is exactly what the cancer center’s staff was aiming for when ground was broken in 2013 on the $26 million facility, said Judy Bekowitz, MSN, RN, OCN, a nurse manager.
The center includes a spacious waiting area with gleaming floors, ambient lighting, and automatic blinds to shield patients who might be sensitive to bright light from the glaring sun. At 25,000 square feet, the space is more than four times as large as the center’s previous location. Patients will also have access in the coming months to a pharmacy kiosk that will allow them to fill prescriptions on site. The number of exam rooms has more than doubled, from six to 20, and there are 21 infusion chairs with mounted television screens where patients receive their intravenous medications.
Bekowitz described the new facility as “a one-stop shop,” allowing patients to fill and pick up prescriptions, build a medical treatment plan in consultation with an array of on-site doctors, and receive treatment without having to shuttle between buildings. “Patients can come here and leave at the end of the day with a complete plan of care,” she said.
Dunford was pleasantly surprised to learn that she would have access to everything she needed to fight cancer in one place. “My oncologist is here, my surgeon is here, and my radiologist too,” she said. “Having all three under the same roof allowed for fast reaction times and allowed the doctors to quickly develop a plan for treatment.”
Before construction, members of the staff conducted extensive research by visiting hospitals in neighboring states, and a team of nurses worked with a designer and an architect to select calming paint colors, mood-altering lighting, and artwork depicting tranquil settings, Bekowitz explained.
Julie Renee Brahmer, MD, director of the cancer center, said that in addition to focusing on the design of the physical space, staff members placed a premium on easing the transition for patients facing various stages of cancer and complicated treatment schedules. “These nurses have gone from zero to 180 mph in order to care for our patients,” she said.
Susan Garriss, who was diagnosed two years ago with breast cancer, believes the new environment has the ability to aid her recovery. “It sounds strange, but I like to come here for my treatment because I love the atmosphere,” said Garriss, who lives in Dundalk and works in sales and marketing. “This place is so cheerful and I’ve made a remarkable recovery,” added Garriss, who’s in her early 60s but said she feels “like I’m in my 20s.”

“This place is so cheerful,” says patient Susan Garris, above with Katherine Schuerholz, RN.
On a recent Friday, as Dunford sat hooked up to an IV, an episode of General Hospital playing in the background, she couldn’t help but feel thankful for the “little things,” like privacy and solitude. At the Norfolk facility where she received treatment last year, “we all couldn’t help but be involved with one another’s sickness. Of course, you want to have empathy for other patients, but you also want to focus on your own individual care too. This environment is helpful for essential well-being.”
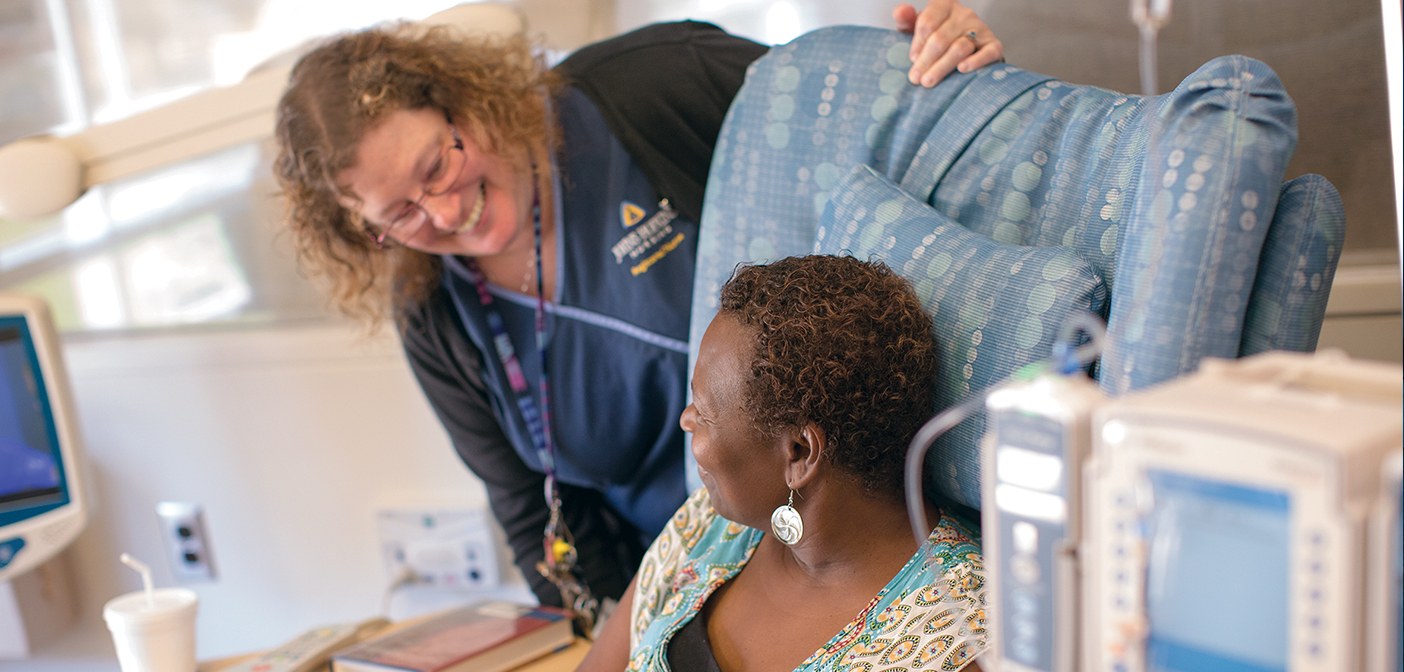
Photos by Chris Hartlove | Photo at top: Barbara Ziegler, RN, and Jacqueline Dunford, who was surprised to find all her caregivers under one roof.
 Forging Policy: How Can Doulas Improve Black Maternal Health?
Forging Policy: How Can Doulas Improve Black Maternal Health? Q & A With Forensic Nurse, Michelle Patch
Q & A With Forensic Nurse, Michelle Patch Guatemala Re-visited: Rainwater Project Shows Value of Service-learning Trips
Guatemala Re-visited: Rainwater Project Shows Value of Service-learning Trips You’re Welcome
You’re Welcome Dr. Robert Atkins, Anna D. Wolf Endowed Professor
Dr. Robert Atkins, Anna D. Wolf Endowed Professor






