By Jennifer L.W. Fink
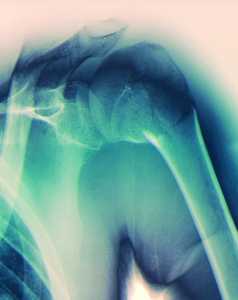
The orthopedic nurses who work in the Sibley Institute of Bone & Joint Health program know that their patients’ experiences begin (and end) outside of the hospital setting. They don’t wait for a patient to show up for surgery to begin the caring process.
Sibley nurses and physicians combine forces to offer an orthopedic seminar series for the public, says Cathy Pulford, nurse practitioner and program coordinator for the Bone & Joint Health program. Sibley nurses also lead pre-operative joint replacement classes for people who will be undergoing the procedure. “We cover, soup-to-nuts, what it’s like to get your joint replaced, what will happen in the hospital the day of surgery, what will happen after surgery, what will happen if you go to the rehab unit, and what will happen when you come home,” says Suzanne Honchalk, nurse navigator.
Pulford and Honchalk talk to patients prior to surgery to determine if they have any special needs that will affect their surgery or recovery. “We want to know if someone has an insulin pump, or if they’ve had a previous stroke and have weakness on one side, or if they have pain management issues and are on narcotics,” Pulford says. “We pull that information together and share it in a weekly multi-disciplinary meeting, so we’re prepared.”
If the pre-assessment reveals a specific need, staff handle the situation proactively. “If someone has underlying dementia, we may talk to the family about having a sitter at the bedside, to watch that person, for safety reasons,” says Christine Inglisa, nurse manager of orthopedics.
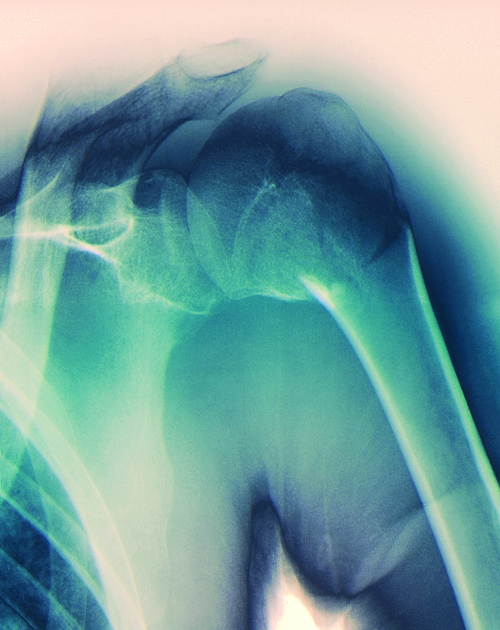
While the Sibley Institute of Bone & Joint Health has long had an excellent reputation, staff members are constantly striving to improve patient satisfaction and outcomes. The team recently pooled efforts to decrease heel ulcers, a common complication after joint surgery.
“One of our front line leaders brought the problem to my attention,” Inglisa says. “Our numbers weren’t bad, but we set a goal to reduce our heel ulcers by 50 percent. We decided we would adopt whatever practices were necessary to prevent heel ulcers, and that we would work toward consistency across the patient continuum.”
Sibley staff now use a specialized pillow to relieve pressure on patients’ heels. Anesthesia practices have been tweaked to allow increased sensation of the heel area. Repositioning is stressed. Heel ulcers have since decreased and patient satisfaction rates have increased. The Institute of Bone & Joint Health hasn’t had an infection in nearly a year.
“We’re a committed team,” Inglisa says. Pulford agrees: “We are in it for the patients, and as long as your focus is always the patients, you can’t do anything wrong.”
 A Letter from Deborah Baker:
A Letter from Deborah Baker: 2019 DAISY Awards
2019 DAISY Awards Nurses and Midwives “Power the Path” to Universal Health Coverage
Nurses and Midwives “Power the Path” to Universal Health Coverage The Unmentionable Vaccine
The Unmentionable Vaccine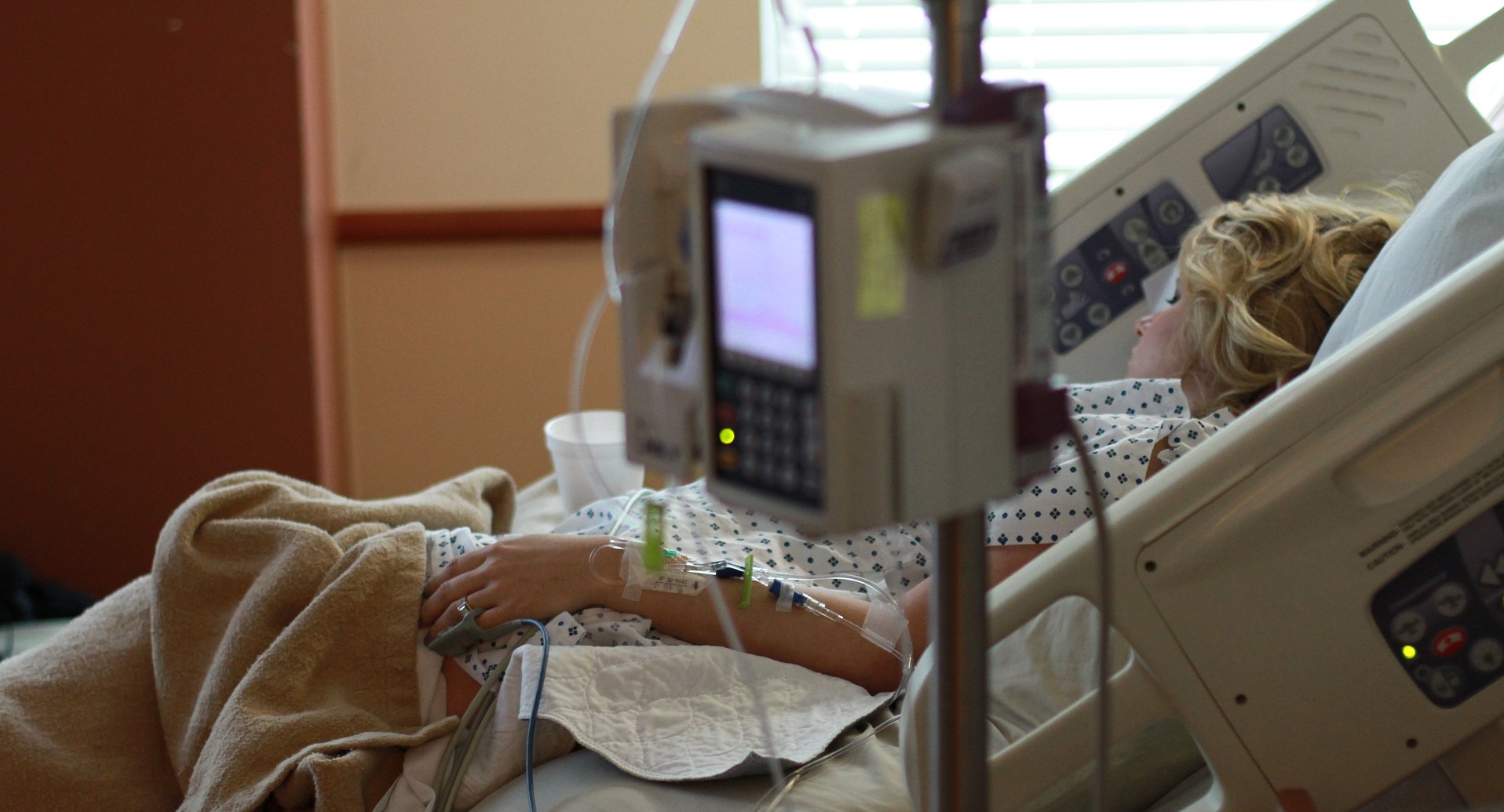 What Nurses Need to Know: Tracheostomy Patients at Home
What Nurses Need to Know: Tracheostomy Patients at Home







