Bayview’s SICU nurses are fighting bloodstream infections
Stephanie Shapiro
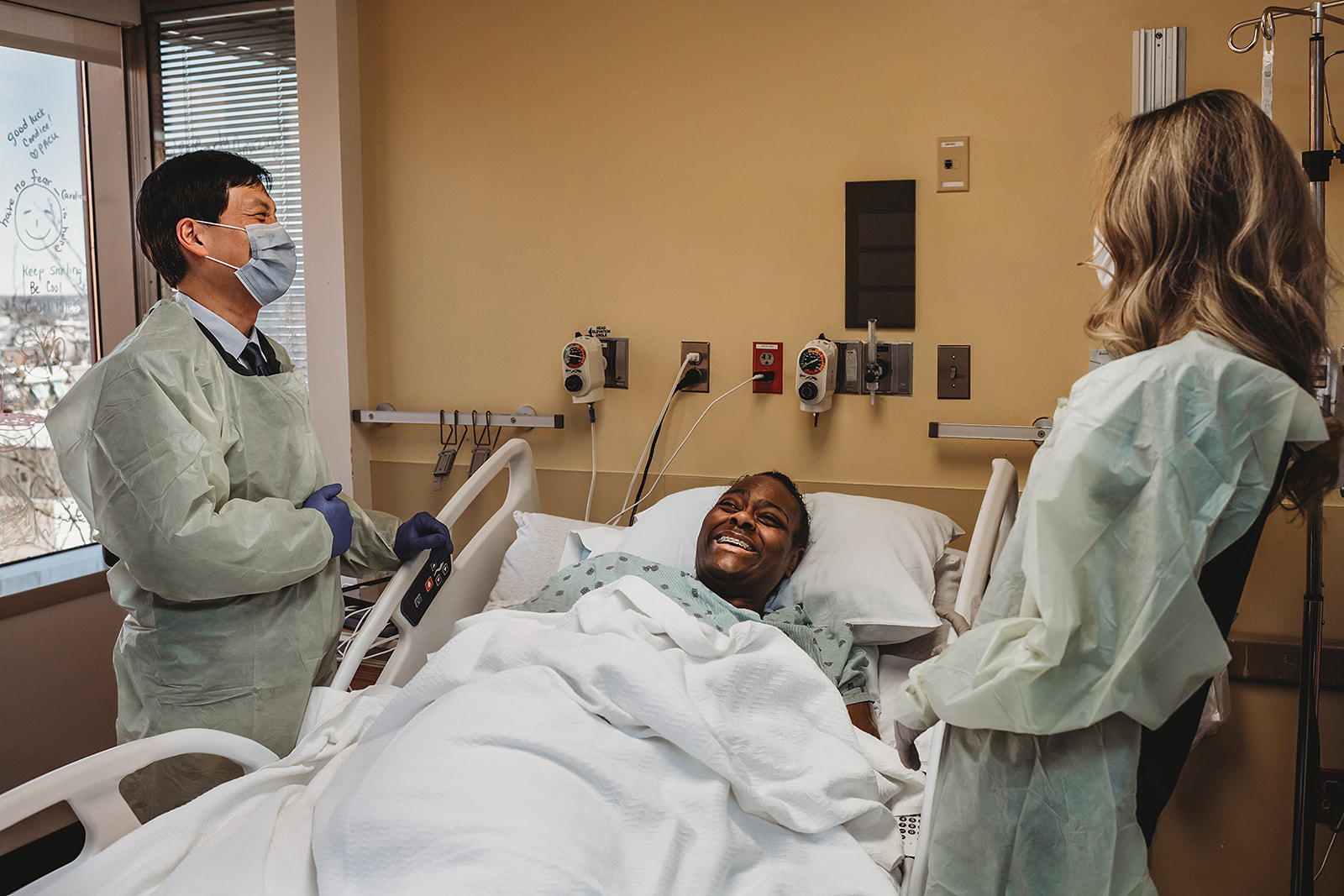
In the Surgical Intensive Care Unit (SICU) at Johns Hopkins Bayview Medical Center, the prevention of blood stream infections demands an arsenal of safety measures, from a unit-based safety officer and Chlorohexidine skin prep to timely line removal and full barrier precautions. But central to that multi-pronged effort is making nurses equal members of the healthcare team, says patient care manager Carol Miller, RN, CCRN. of the previous year’s average of 3.29 infections per 1,000 central line days.

To prove her point, Miller points to a remarkable record: In 2008, her unit reported no central line catheter-related infections, a feat that came on the heels of the previous year’s average of 3.29 infections per 1,000 central line days.
Ultimately, the units infection-free record extended to 704 days in a row, giving Miller and Zeina Khouri-Stevens, PhD, RN, bragging rights to “SICU Pride” during a poster presentation at last year’s Maryland Patient Safety Conference.
Miller also gives kudos to “our physician assistants and nurse practitioners who place the majority of the lines. They have been extremely vital to this whole process.”
Over the years, Miller has witnessed her unit’s shift to a culture that prizes safety over hierarchy. “You could have a checklist and make the marks, but you also have to empower the staff to stop a procedure if they see something is not going right,” she says. “That takes a lot of work.”
The unit’s commitment to eliminating central line infections “took a big push forward” when the SICU became part of the Johns Hopkins program, “Partnerships and Interventions to Promote and Ensure Patient Safety,” says Miller. The alliance lends support and reaffirms the guiding principle of the unit’s safety-first culture that she sums up as, “We all are accountable for providing this higher level of safety for our patients.”
In the Hopkins Bayview SICU, nurses are encouraged to think critically and make clinical decisions. They don’t hesitate to stop a procedure if sterile practices aren’t followed, Miller says. On occasion, she, too, has intervened in ways once thought unimaginable. “I’ve caught providers before they actually enter a room to assist with a sterile procedure and reminded them to put on a mask and other protective gear,” Miller says.
That’s a far cry from her early years on the SICU, when “nurses just followed orders and didn’t question,” she says. Today, “the culture truly is a team effort. The physician may ultimately have the final say, but the nurse or any member of the team can step out and say, ‘Let’s talk about it.’ We work like that now, and I think our infection-free success is a reflection of that.”
 ‘Helpful, Powerful, Kind’ Palliative Care
‘Helpful, Powerful, Kind’ Palliative Care Researchers to Enter Sigma Hall of Fame
Researchers to Enter Sigma Hall of Fame What We Know About the Coronavirus
What We Know About the Coronavirus What Nurses Don’t Know on CLABSI
What Nurses Don’t Know on CLABSI Summer Research 2019
Summer Research 2019







