Originally published in Dome, September 2008.
The nation’s first ICU emerged at Johns Hopkins Bayview 50 years ago.
A half-century ago, the offer of $150 to participate in a potentially harrowing medical experiment at the old Baltimore City Hospital, now Johns Hopkins Bayview Medical Center, was something third-year medical student Chester Schmidt Jr. felt was too good to turn down-even if it meant being injected with a drug that briefly paralyzed his diaphragm. “That was a lot of money then,” he recalls with a chuckle.
Schmidt, later the long-time director of psychiatry at Johns Hopkins Bayview, volunteered to let Peter Safar (1924-2003), then head of anesthesiology at City Hospital, use him as a guinea pig to test his new, groundbreaking methods for cardiopulmonary resuscitation. Such experiments, which subsequently earned Safar recognition as the “father of CPR,” were among the astonishing innovations in critical care medicine that he initiated at City Hospital–including the opening in September 1958 of the country’s first multi-disciplinary intensive care unit (ICU).
Since July, each of Johns Hopkins Bayview ‘s six ICUs–medical, surgical, coronary, neonatal, neuroscience and burn–individually has celebrated the 50th anniversary of their prototype’s creation and their own unique contributions to that heritage. The celebration culminated on September 26th with a day-long symposium at Johns Hopkins Bayview, featuring lectures by some of the premiere physicians in critical care medicine from around the country.
Philip Zieve, former head of Johns Hopkins Bayview’s department of medicine and chief of the center’s medical staff, was an intern at City Hospital when the ICU was founded. He recalls Safar as an “aggressive and charismatic” leader of anesthesiology “who believed that there was an opportunity for better respiratory care if the patients could be hospitalized in a single unit with nurses trained to care for people with severely acute problems.”
At the time, City Hospital was Baltimore’s major polio center, but once the Salk vaccine virtually ended the threat of polio, Safar saw the opportunity to transform the hospital’s four-bed ventilator unit into an ICU, Zieve says. It had round-the-clock staffing by an anesthesiologist, nurses and a surgeon, says Romergryko Geocadin, director of Johns Hopkins Bayview’s neuroscience CCU, and became “the template for what the ICU today looks like.”
The first ICU had just six beds, Zieve recalls. At today’s 709-bed Johns Hopkins Bayview, one of every six beds is in an ICU, says [Jonathan] Sevransky [head of medical ICU]. Last fiscal year, 5,941 ICU patients were treated there.
 |
| Nurses in the ICU at Johns Hopkins Bayview Medical Center carry on 50-year legacy, begun when the nation’s first ICU emerged at their hospital. |
In the Hopkins Hospital’s nine ICUs–neonatal, pediatric, cardiac surgical, surgical, medical, neuro critical care, coronary care, oncology and Weinberg–nearly 10,000 patients are treated annually, says Todd Dorman, vice chair for critical care. About 20 percent of the hospital’s 1,017 beds are in ICUs, he adds.
Today, hundreds of nurses and dozens of physicians, respiratory therapists, pharmacists and support personnel work in the two hospitals’ ICUs.
With people surviving longer with serious illnesses, “it’s likely that hospitals will become more and more devoted to patients who need life support,” Sevransky says. It is estimated that one percent of the country’s gross domestic product already is being spent on ICU care, he notes.
“At the end of the day, after all the hoopla,” says Geocadin, “if we can rekindle the zest of Peter Safar when he was at Johns Hopkins Bayview creating all of this, it will inspire people.”
-Neil A. Grauer
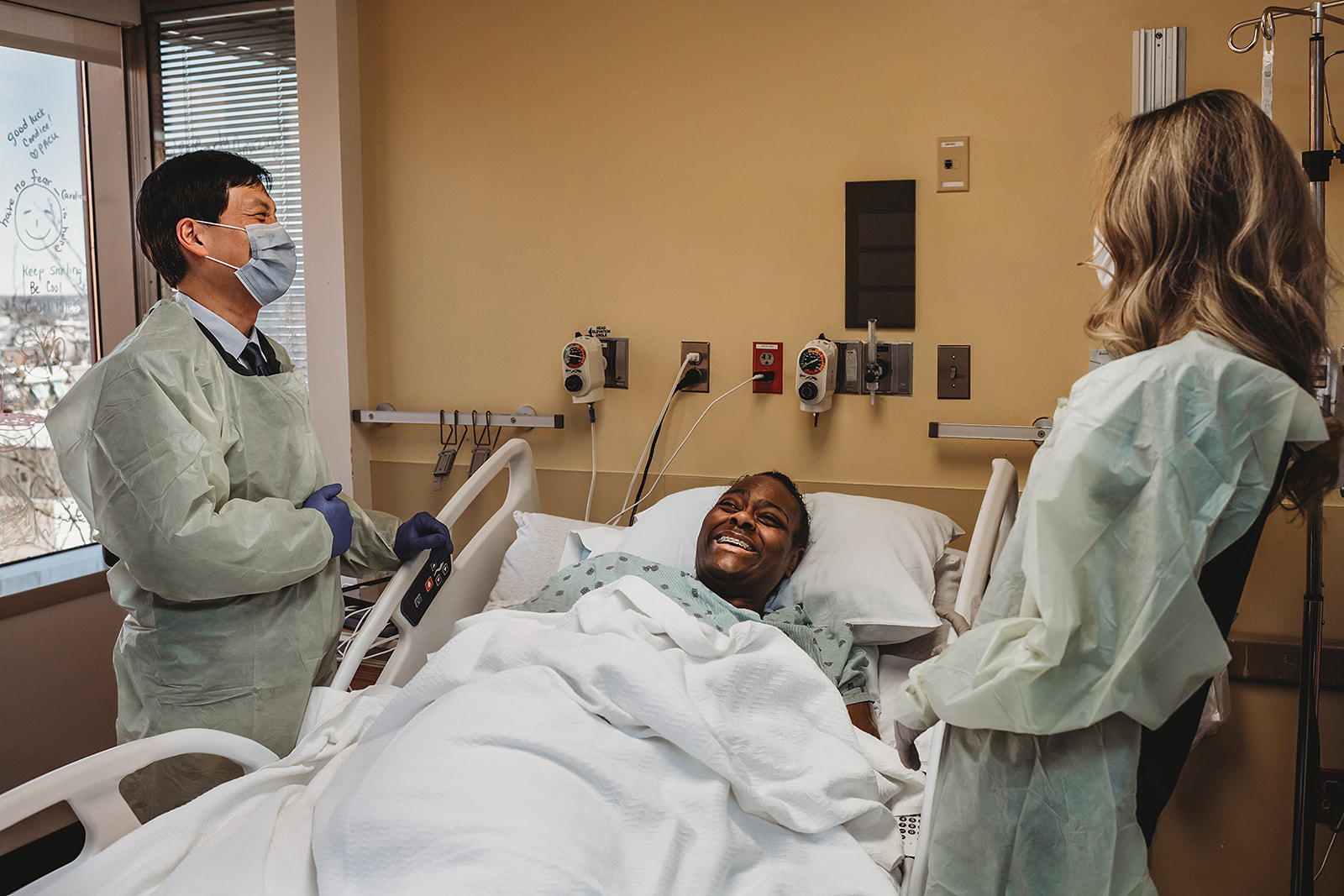 ‘Helpful, Powerful, Kind’ Palliative Care
‘Helpful, Powerful, Kind’ Palliative Care Breaking Barriers
Breaking Barriers Pregnant Pause
Pregnant Pause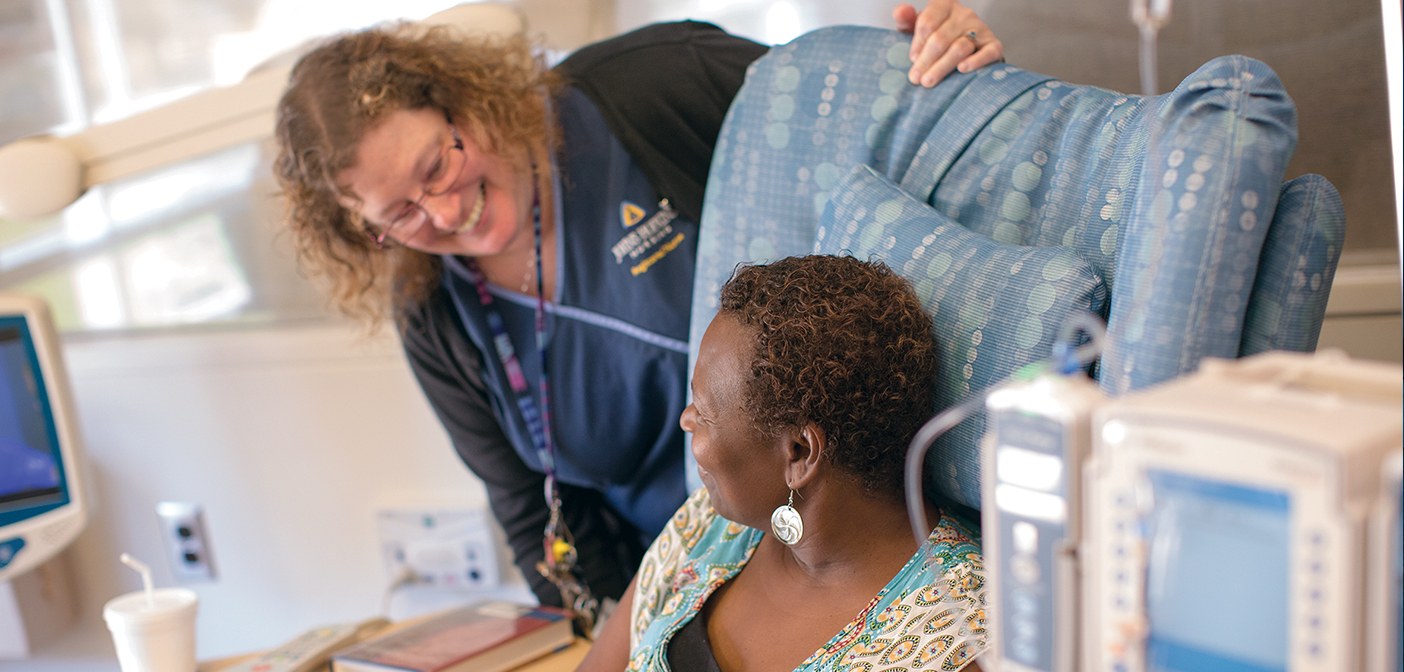 In Your Own World
In Your Own World Bayview’s Journey of Improvement
Bayview’s Journey of Improvement







