The Heart of Suburban’s Universal Bed Mode
by Susan Middaugh
![]() When caring for patients planning open heart surgery, establishing the right tone, staff, and setting are important. “They’re scared, and their families are scared,” says Kimberley Kelly, MBA, RN, CCRN, nursing director of critical care at Suburban Hospital.
When caring for patients planning open heart surgery, establishing the right tone, staff, and setting are important. “They’re scared, and their families are scared,” says Kimberley Kelly, MBA, RN, CCRN, nursing director of critical care at Suburban Hospital.
With compassion as the starting point, Suburban has taken an unusual approach to preparing cardiac surgical patients for recovery. Since the NIH Heart Center at Suburban Hospital opened six years ago, patients receive all of their care on one unit—a prac-tice called the Universal Bed Model.
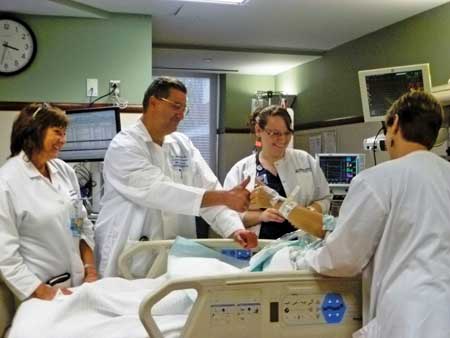
“A team of versatile nurses have to be highly skilled to handle the acute critical care needs of the patient. At Suburban, we adjust our staffing ratios according to the patient’s clinical needs,” explains Kelly.
“This approach is seamless for the patient and gratifying for the nurses,” adds Linda Krause, MSN, ACNP, FNP, RN, CSC, one of three acute care nurse practitioners for cardiothoracic surgery at the Center.
Clinical educator Sarah Rasmussen, MSN, RN, CCRN, notes that when patients and their families come in for pre-operative orientation, the first thing nurses do is introduce themselves. “There is a consistency and continuity of care,” she says.
Patients and their loved ones find the continuity comforting. Montgomery County Circuit Court Judge Durke G. Thompson recalls his experience as a patient at the Center: “It gave me peace of mind. I got to know my care team, but more important, my care team got to know me.”
Moreover, the Universal Bed Model is having a positive impact on quality of patient care and outcomes. According to the Society of Thoracic Surgery, from May 2006 through December 2010 the risk-adjusted mortality rate was lower at Suburban (1.6 percent) than the national average (2.2 percent). The median post-operative length of stay for coronary artery bypasses was also better at Suburban (5 days) than nationally (7 days), and the readmission rate was lower (6.7 percent vs. 10.1 percent).
“Because our approach is unusual, we seek a different kind of critical care nurse with abilities that run deeper,” says Kelly. Finding the “right” nurses for the Heart Center can be challenging.
Rasmussen agrees. At the Heart Center, “our nurses have to be prepared to care for patients with changing acuities, ranging from a 1:1 patient ratio during their immediate post-operative period to a 1:4 assignment with patients who are ready for discharge. They have to be more nimble.” To prepare, nurses undergo several weeks of training to enhance their critical care thinking skills. It is a challenge Rosemarie Gurion, RN, welcomed when she joined the Heart Center in 2006—a year after graduating from nursing school. It was her second profession, and she wanted to make sure it was the right fit. Although she has worked as an intensive care unit nurse, Gurion says she prefers the Universal Bed Model because “I’m connected to my patients from orientation to discharge.”
 DAISY Awards Fall 2023
DAISY Awards Fall 2023 A Letter from Deborah Baker: The Role of Your Career, Right Here
A Letter from Deborah Baker: The Role of Your Career, Right Here Heart Health in Native Populations
Heart Health in Native Populations Summer Research Roundup 2023
Summer Research Roundup 2023 Sky’s The Limit
Sky’s The Limit







